TL;DR:
- Therapy resistance is a medical condition, not a personal flaw or lack of effort.
- Up to 30% of depression cases are treatment resistant, often linked to biology and trauma.
- Personalized, trauma-informed approaches can break through therapy resistance and improve outcomes.
Up to 30% of people with major depressive disorder try multiple treatments and still don’t feel better. If that sounds like you, you are not broken, lazy, or beyond help. Therapy resistance is a medically recognized condition that has nothing to do with how hard you’re trying or how much you want to heal. This guide unpacks what therapy resistance actually is, who experiences it, why it happens at a biological level, and what concrete steps you can take right now to move toward real relief.
Table of Contents
- What is therapy resistance? Definitions and myths
- Who is affected by therapy resistance and why?
- Why therapy resistance happens: underlying causes
- First steps: what to do when therapy isn’t working
- Why most people misunderstand therapy resistance and what actually matters
- Personalized help for therapy resistance: your next chapter
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Therapy resistance is real | About one in four people with depression may face therapy resistance even after trying multiple treatments. |
| Multiple causes exist | Genetics, trauma, and medical factors can all contribute to resistance—not just motivation or effort. |
| Actionable steps help | Ruling out pseudoresistance and seeking new professional input can open doors to progress. |
| Personalized care matters | Tailored, trauma-informed approaches are crucial for overcoming resistance and achieving mental health goals. |
What is therapy resistance? Definitions and myths
Therapy resistance gets misunderstood more often than almost any other mental health concept. People assume it means someone is being difficult, refusing to open up, or not doing the inner work. None of that is accurate.
From a clinical standpoint, treatment-resistant depression is defined as inadequate response to at least two adequate trials of antidepressant medications at optimal dose and duration, typically six to eight weeks each, despite adherence. The same standard applies to therapy: if you’ve completed multiple full courses of evidence-based treatment and your symptoms persist, clinicians consider that true resistance. It’s a medical status, not a moral judgment.
“Therapy resistance is not a personality flaw. It is a signal that the current approach has not yet matched the underlying biology, history, or complexity of the person’s condition.”
This distinction matters enormously. When people believe they are personally failing therapy, they often stop trying altogether. That decision can cost years of potential healing.
Common myths about therapy resistance:
- It means you’re not trying hard enough
- It only happens to people who aren’t honest with their therapist
- It means you’ll never get better
- It’s the same thing as simply not liking your therapist
- It only affects severe or complicated cases
These myths cause real harm. They delay diagnosis, increase shame, and push people away from trauma recovery options that could genuinely help.
Therapy resistance vs. normal treatment hurdles:
| Factor | Normal treatment hurdle | True therapy resistance |
|---|---|---|
| Duration | Brief plateau or rough patch | Persistent symptoms across full treatment courses |
| Response | Some improvement over time | Little or no meaningful improvement |
| Cause | Adjustment period or life stress | Biological, genetic, or complex psychological factors |
| Treatment | Stay the course | Requires reassessment and alternative approaches |
| Blame | Situational | Medical, not personal |
Understanding this difference is the first step toward seeking the right evidence-based depression solutions and getting proper support.
Who is affected by therapy resistance and why?
With the definition established, it’s critical to understand who experiences therapy resistance and the factors that increase vulnerability. The answer might surprise you: therapy resistance touches people of every age, income level, background, and level of motivation.
TRD affects 20 to 30% of individuals with major depressive disorder. That’s roughly one in four people diagnosed with depression who won’t find adequate relief through standard first and second-line treatments. In a state as large and diverse as California, that represents hundreds of thousands of people who are still searching for answers despite doing everything “right.”
Who carries the highest risk?
- People with a history of childhood trauma or adverse childhood experiences (ACEs)
- Individuals with a family history of depression or treatment resistance
- Those with co-occurring anxiety, PTSD, or chronic pain conditions
- People dealing with chronic stress from poverty, discrimination, or housing instability
- Individuals with certain genetic variations affecting how they process medication
- Women, who statistically show different biological responses to some antidepressants
Risk factors by category:
| Category | Risk factor | Impact on resistance |
|---|---|---|
| Genetic | Serotonin transporter gene variants | Reduces medication response |
| Psychological | Unresolved childhood trauma | Increases severity and duration |
| Medical | Chronic inflammation or thyroid dysfunction | Mimics or worsens depression |
| Social | Ongoing stressors such as poverty or trauma exposure | Limits treatment gains |
| Developmental | Early adversity during brain development | Alters mood regulation circuits |
Trauma history deserves special attention. Research consistently shows that people who experienced early adversity have a higher likelihood of developing not just depression, but depression that resists standard care. This is why understanding the importance of childhood therapy early is so valuable. When children receive appropriate support, it can reduce the long-term risk of treatment-resistant patterns developing later in life.
The connection between early trauma and holistic trauma recovery approaches also highlights why standard medication alone rarely tells the full story for many people.
It is also worth knowing that teenagers are not immune. Young people going through developmental changes, academic pressure, or family dysfunction can develop patterns of depression that are harder to treat, especially if underlying trauma or genetic vulnerability is present. Looking into child therapy steps early can make a measurable difference in long-term outcomes.
One important takeaway: therapy resistance is not a character weakness. It reflects the intersection of biology, personal history, and circumstances that are often completely outside of a person’s control.
Why therapy resistance happens: underlying causes
Now that we know who’s at risk, it’s important to uncover the science of why therapy resistance can persist despite best efforts. The mechanisms are real, measurable, and increasingly well understood.
The biological roots of therapy resistance are complex. Genetic polymorphisms, including variations in the SLC6A4 serotonin transporter gene, affect how efficiently the brain processes serotonin. People with certain variants absorb or recycle serotonin differently, which means standard SSRI medications may work poorly or not at all. This isn’t something you can will away through effort.
Inflammation is another major driver. Elevated levels of cytokines such as TNF-alpha and IL-6, both markers of chronic immune system activation, have been linked to depression that doesn’t respond to typical treatments. People with high baseline inflammation often have brains that behave differently under stress and recover more slowly from emotional injury.
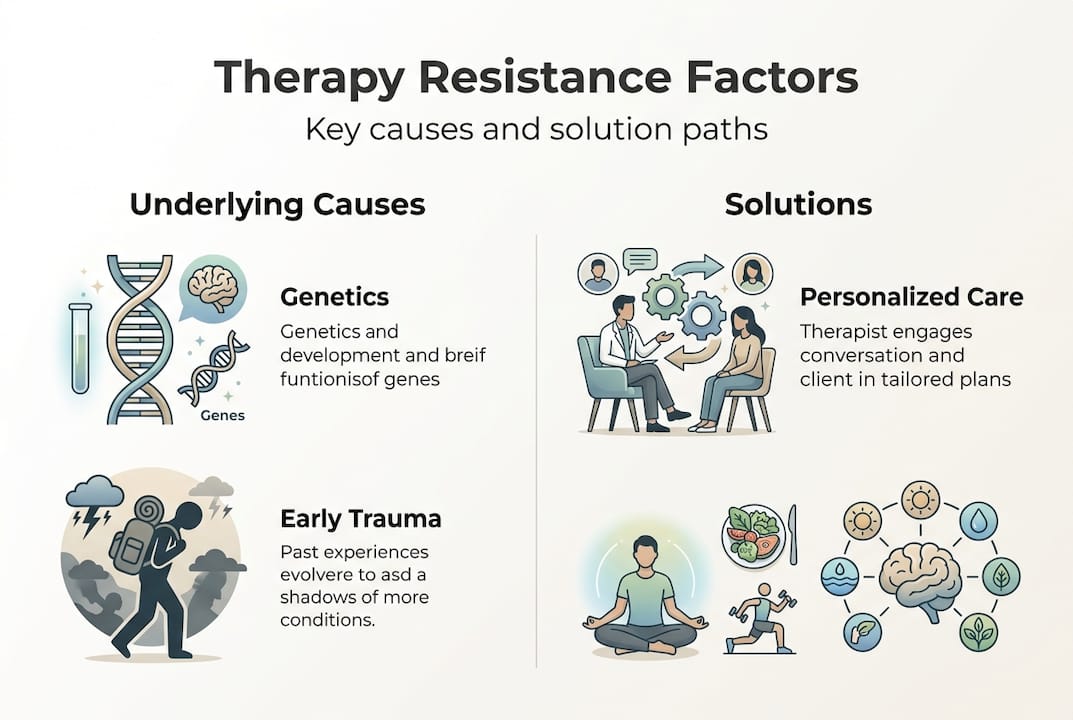
The main biological and psychological causes of therapy resistance:
- Genetic factors: Specific gene variations alter how neurotransmitters like serotonin and dopamine are processed, making standard medications less effective for some people.
- Chronic inflammation: Persistent immune system activation changes how brain circuits involved in mood, motivation, and reward function over time.
- Neuroplasticity deficits: The brain’s ability to form new connections is reduced in some cases of resistant depression, making it harder to benefit from talk therapy or behavioral interventions.
- Early life adversity: Trauma during childhood can literally rewire the brain’s stress response system, the HPA axis, leaving it in a state of chronic over-activation that medication alone often can’t reverse.
- Sex-based differences: Hormonal and neurological differences mean that men and women can respond very differently to the same treatment, and these differences are often underestimated in clinical settings.
- Comorbid conditions: When anxiety, PTSD, or a personality disorder exists alongside depression, each condition can worsen the other and make standard treatments less effective.
Early life adversity is worth pausing on. When a child grows up in an environment of abuse, neglect, or chronic unpredictability, the brain adapts to survive that environment. The stress circuits become hyperactive. The emotional regulation centers develop differently. These are not metaphors. They are structural and functional changes that persist into adulthood and explain why CBT and resistance can be more complicated for trauma survivors than for someone without that history.
Mindfulness for resistance has emerged as a valuable complement to other treatments precisely because it works at the level of the nervous system, calming the hyperactivated stress response rather than just addressing thought patterns.

Pro Tip: If your progress has stalled, ask your provider to specifically assess for undiagnosed trauma, inflammatory conditions, or genetic factors. This conversation could change the entire direction of your care and has nothing to do with how motivated or cooperative you are.
First steps: what to do when therapy isn’t working
Knowing why therapy resistance happens leads directly to what actions you can take for meaningful change. If you feel stuck, the worst thing you can do is assume the problem is you. The second worst thing is to stop trying entirely. Here is a practical sequence of steps.
Pseudoresistance must be ruled out first: this means checking for inadequate dosing, not staying in treatment long enough, inconsistent adherence, comorbid conditions, misdiagnosis, or pharmacogenetic issues that affect how your body processes medication. A surprising number of people who appear to be treatment resistant are actually experiencing pseudoresistance, where the treatment was technically adequate on paper but not truly optimized for their specific situation.
Step-by-step plan when therapy isn’t working:
- Review your current treatment honestly. Are you taking medication consistently? Are you attending sessions regularly? Have circumstances changed that might explain why things feel worse? Rule out the basics before assuming true resistance.
- Ask your provider directly about pseudoresistance. Not all clinicians bring this up proactively. Ask them to review your medication doses, duration, and adherence history with fresh eyes.
- Seek a second opinion. This is not disloyal to your current provider. Getting another perspective from a psychiatrist, psychologist, or specialized clinician can reveal missed diagnoses or overlooked factors.
- Request a deeper assessment. Ask about genetic testing (pharmacogenomic testing) that shows how your body metabolizes common psychiatric medications. This is more widely available now and can dramatically change medication decisions.
- Explore alternative or additional treatment approaches. Different modalities of therapy, such as EMDR for trauma, acceptance and commitment therapy (ACT), or dialectical behavior therapy (DBT), may work when standard CBT has not. Medication adjustments, augmentation strategies, or newer interventions may also be worth discussing.
- Look into integrated care. Sometimes combining therapy, medication, lifestyle interventions, and peer support creates results that none of those approaches achieves alone.
Exploring all your therapy options in California means understanding that care is not one-size-fits-all. The right combination for you may look very different from what worked for a family member or friend.
Pro Tip: Start a detailed symptom journal between sessions. Track your mood, sleep, energy, appetite, and any life events daily. Over several weeks, patterns will emerge, including triggers, cycles, and times of day when symptoms peak. This data is genuinely useful to your provider and often points to overlooked causes.
Why most people misunderstand therapy resistance and what actually matters
Here is something that most mental health content gets wrong: therapy resistance is framed as a problem with the patient. It is actually a problem with the match between the treatment and the person.
We’ve worked with clients who spent years trying the same type of talk therapy, seeing marginal improvements, and concluding they were simply beyond help. When they finally received trauma-informed care that addressed the root causes of their resistance, including childhood adversity and its neurological effects, things began to shift. Not overnight, and not without effort. But they shifted.
Childhood trauma increases TRD risk and severity, and may even reduce the efficacy of newer interventions like ketamine. The inflammation links suggest that targeted approaches, including anti-inflammatory strategies and trauma-specific therapies, may be more effective for this population. This is exactly why matching treatment to the root cause matters more than repeating the same approach and hoping for a different result.
The most important shift we see in clients who eventually break through therapy resistance is this: they stop blaming themselves and start advocating for a different approach. That advocacy looks like asking hard questions, requesting assessments, seeking second opinions, and refusing to accept “treatment resistant” as a permanent identity rather than a temporary clinical status.
Therapy’s impact on trauma is well documented, but the type of therapy matters enormously. EMDR, somatic approaches, and trauma-focused CBT all work at different levels of the nervous system than standard talk therapy. For people with complex trauma histories, these distinctions are not minor details. They are the difference between progress and stagnation.
Variety and customization are not luxuries. They are clinical necessities for anyone who has not responded to standard care. If your treatment plan has looked the same for two or more years without meaningful change, that’s a signal worth acting on, not a reason to give up.
Personalized help for therapy resistance: your next chapter
Understanding what drives therapy resistance is only valuable if it leads you to better care.
At Revive Health Therapy, we work with Californians who haven’t found relief through standard treatment. Our approach centers on trauma-informed therapy benefits and individualized assessment, which means we look at your full history, biology, and circumstances before deciding on a path forward. Whether your struggle involves depression, anxiety, trauma, or complex combinations of all three, our team uses methods like EMDR, CBT, and mindfulness to target what’s actually driving your resistance. We offer both in-person sessions in Walnut Creek and Oakland and secure telehealth across California, with sliding-scale fees and insurance options. Learn more about our depression treatment options or explore why psychotherapy works as a starting point. You deserve care that’s built around you.
Frequently asked questions
How do I know if I’m therapy resistant?
Therapy resistance is often identified when you show little or no improvement after two complete, adequate treatment attempts, even with consistent adherence and proper dosing. If you’ve met that threshold, treatment-resistant depression is a clinical label worth discussing with your provider, not a life sentence.
What are common signs of pseudoresistance?
Pseudoresistance typically involves missed doses, leaving treatment before it has had adequate time to work, an underlying misdiagnosis, or unmanaged medical conditions like thyroid dysfunction that mimic or worsen depression symptoms.
Does trauma make therapy resistance more likely?
Yes. Childhood trauma increases TRD risk and severity, meaning people with adverse early experiences are statistically more likely to need specialized, trauma-focused care rather than standard first-line treatments.
Can therapy resistance be overcome?
Most people do find meaningful progress with the right combination of thorough assessment, tailored treatment, and sometimes a mix of modalities. Treatment-resistant depression is a challenging condition, but it is not a permanent one for the majority of people who receive specialized care.
Is therapy resistance common in California?
The prevalence is consistent with national data: roughly 20 to 30% of people diagnosed with major depression experience therapy resistance, which means it affects a very large number of Californians across all demographics and regions.
Recommended
- Defining therapy outcomes: clear measures for real progress – Revive Health Therapy
- Step by step therapy guide for Californians 2026 – ReviveHealthTherapy
- Group therapy explained: methods, effectiveness & what to expect – Revive Health Therapy
- Therapy for Teens: Building Self-Growth and Resilience – ReviveHealthTherapy