TL;DR:
- Depression is a treatable medical condition, not a character flaw or weakness.
- A structured, evidence-based workflow improves recovery chances through standardized assessment and therapy.
- Telehealth and affordable programs like Medi-Cal expand access to effective depression treatment in California.
Depression is not a character flaw or a sign of weakness. It is a medical condition that affects roughly 1 in 5 California adults at some point in their lives, and the good news is that structured, evidence-based approaches work. What separates people who recover from those who stay stuck is rarely willpower. It is having a clear, practical roadmap built on proven methods. This guide walks you through exactly that: a step-by-step workflow grounded in the same clinical standards therapists use every day, including tools covered by Medi-Cal and accessible across California whether you are in San Francisco, Fresno, or anywhere in between.
Table of Contents
- Understanding depression: The starting point in California
- Step-by-step workflow: From first symptoms to recovery
- Personalizing your depression workflow: California access and adaptations
- Troubleshooting and special cases: When the workflow needs adjustment
- What most guides miss: The crucial mindset for success
- Get expert guidance for your next step
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Follow a proven workflow | Structured, evidence-based steps give you the best chance at steady progress and recovery. |
| Monitor and adjust early | Track symptoms by week 4 and change approach promptly if needed for the best results. |
| Personalize for better outcomes | Tailor therapies and access methods to your needs, using California’s abundant resources. |
| Accessible support in California | Medi-Cal and community options make high-quality depression treatment affordable and attainable. |
Understanding depression: The starting point in California
One of the biggest barriers to getting help is not knowing where to begin. Depression can feel like a fog that makes every decision harder, including the decision to seek treatment. That confusion is real, and it is also one of the reasons a structured workflow matters so much. Instead of guessing what might help, you follow a sequence that therapists and physicians have refined over decades.
Depression is a treatable medical condition, not a permanent state. The evidence-based depression treatment landscape includes psychotherapy, medication, lifestyle interventions, and combinations of all three. Research confirms that an evidence-based workflow for overcoming depression involves initial screening with the PHQ-9, thorough assessment, personalized treatment planning, progress monitoring, and timely adjustments if improvement stalls.
The PHQ-9 is a nine-question self-report tool that scores depression severity from 0 to 27. It gives you and your therapist a concrete baseline number to track over time. That number is not a label. It is a starting point.
Here is what the PHQ-9 score ranges mean in practice:
| PHQ-9 Score | Severity Level | Recommended Action |
|---|---|---|
| 0 to 4 | Minimal | Monitor, self-care strategies |
| 5 to 9 | Mild | Watchful waiting, lifestyle changes |
| 10 to 14 | Moderate | Begin therapy or counseling |
| 15 to 19 | Moderately severe | Therapy plus possible medication |
| 20 to 27 | Severe | Immediate professional evaluation |
For Californians worried about cost, access is better than many people realize. Medi-Cal covers evidence-based therapies including CBT for eligible adults, and county mental health programs fill gaps for those who do not qualify. You can explore your Medi-Cal options through the Department of Health Care Services.
Key things to know before you start:
- Depression is medical, not moral. Seeking treatment is the same as treating diabetes or high blood pressure.
- Screening is free and fast. The PHQ-9 takes under five minutes and is available through your primary care provider.
- Medi-Cal and county programs cover a wide range of mental health services for qualifying adults.
- Structured workflows replace guesswork with stepwise, measurable progress.
“The greatest mistake in treating depression is waiting for motivation to appear before taking action. The workflow creates the conditions for motivation to return.”
Step-by-step workflow: From first symptoms to recovery
With the foundation in place, here is how the workflow actually unfolds. Think of it as a sequence, not a checklist you complete once and forget.
Step 1: Screen and assess. Complete the PHQ-9 with a provider or therapist. Discuss your history, symptoms, and any prior treatment. This shapes everything that follows.
Step 2: Build a personalized plan. Your therapist works with you to choose the right therapy type, set realistic goals, and decide on session frequency. No two plans look identical.

Step 3: Begin therapy and engage actively. CBT for depression is the most widely studied approach, with an effect size greater than 0.94 and 60 to 70% success rates across 12 to 20 sessions. Sessions are not passive. You will practice skills between appointments.
Step 4: Complete between-session work. Behavioral activation, thought records, and mood tracking are examples of homework that reinforce what happens in session.
Step 5: Monitor progress at week 4. A 20% reduction in PHQ-9 score by week 4 is the clinical benchmark. If you hit it, continue the plan. If not, it is time to reassess.
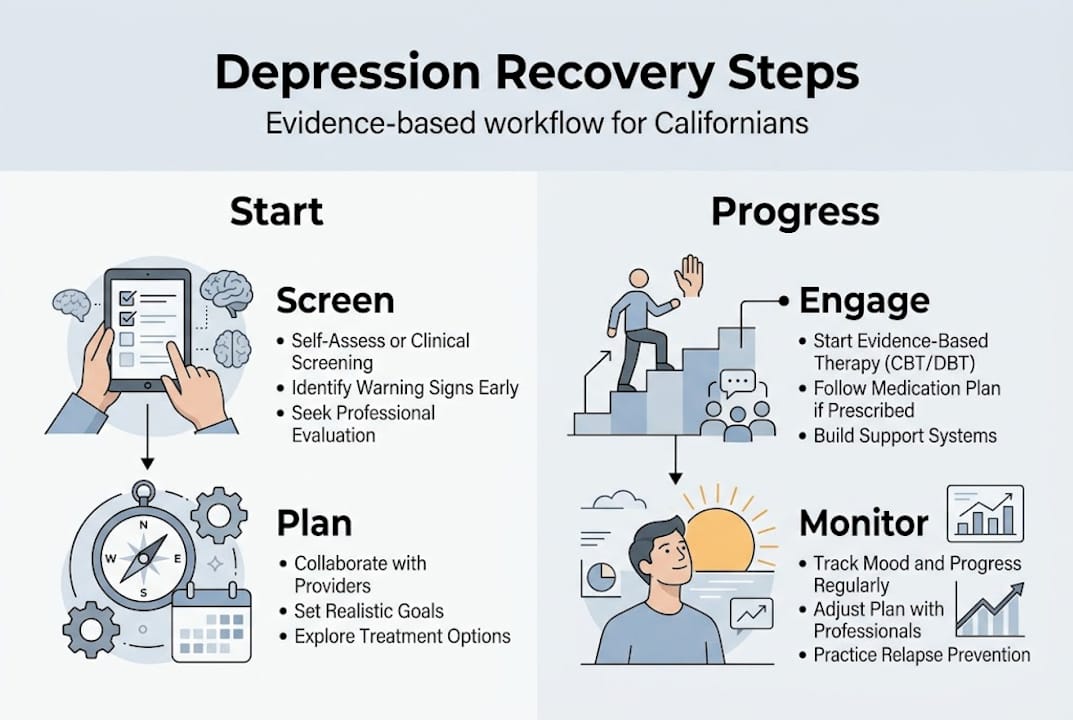
Step 6: Evaluate and adjust. Reliable improvement occurs for 65 to 79% of people by session 12 using validated measures. If you are not in that group, that is not failure. It is information.
Here is a quick comparison of the three most common evidence-based approaches:
| Therapy Type | Best For | Typical Duration | Key Feature |
|---|---|---|---|
| CBT | Most adults | 12 to 20 sessions | Thought and behavior change |
| IPT | Relationship or grief issues | 12 to 16 sessions | Interpersonal skill building |
| Medication | Moderate to severe cases | Ongoing with review | Neurochemical support |
You can review CBT research showing its consistent effectiveness across diverse populations.
Pro Tip: Bring your PHQ-9 scores to every session. Watching the numbers shift over time is one of the most motivating things you can do, and it helps your therapist catch problems early.
The structured therapy steps outlined here are not arbitrary. They reflect decades of clinical trials and real-world outcomes.
Personalizing your depression workflow: California access and adaptations
The standard workflow is a starting point, not a rigid prescription. California’s size, diversity, and range of resources mean that how you access care and which tools you use can vary significantly from someone else’s path.
For many adults, telehealth has changed the equation entirely. If you live in a rural county, work long hours, or have childcare responsibilities, commuting to an office for weekly therapy can feel impossible. Digital and telehealth options remove that barrier. Medi-Cal covers evidence-based therapies through telehealth, and digital tools have been shown to improve adherence and expand reach to underserved communities.
You can check your insurance and telehealth access options before your first appointment so there are no surprises.
How to access low-cost or no-cost care in California:
- Medi-Cal: Apply through Covered California or your county office. Covers CBT, IPT, and medication management.
- County mental health plans: Each California county operates a mental health plan for Medi-Cal beneficiaries. Call 211 for local referrals.
- Sliding-scale private practices: Many therapists, including those at Revive Health Therapy, offer fees based on income.
- HSA and FSA accounts: If you have employer benefits, therapy is typically an eligible expense.
- Federally Qualified Health Centers (FQHCs): Offer integrated behavioral health at reduced cost.
Pro Tip: Before your first session, ask the provider directly: “Do you accept Medi-Cal or offer a sliding scale?” Most therapists will answer honestly, and it saves time for both of you.
For specific populations, therapy type matters. IPT tends to work better for perinatal depression and older adults dealing with grief or social isolation. CBT is the most versatile option for most working-age adults. The California guidelines from the Department of Health Care Services outline which modalities are covered and recommended for different populations.
You can also explore mental health tips tailored specifically for Californians navigating the state’s unique pressures, from wildfire stress to cost-of-living anxiety.
Troubleshooting and special cases: When the workflow needs adjustment
Not every path through depression is linear. Roughly 20 to 30% of people do not respond adequately to their first treatment approach, and that is not a reason to give up. It is a signal to troubleshoot.
Here is how to handle a stalled workflow:
- Identify the stall point. Are you attending sessions but not completing between-session work? Is the therapy type a poor fit? Is there an untreated comorbidity like anxiety or substance use?
- Talk to your provider honestly. Therapists cannot adjust what they do not know about. Share what is and is not working.
- Switch or augment. If CBT is not producing results by week 8, switching to IPT or adding medication is a standard next step, not a setback.
- Consider integrated care. For complex cases involving substance use, chronic pain, or trauma, integrated care research shows that combining behavioral health with primary care produces significantly better outcomes.
- Seek a specialist referral. Treatment-resistant depression may benefit from approaches like EMDR, intensive outpatient programs, or psychiatric evaluation.
“Non-response is not failure. It is diagnostic information that points toward a better-matched treatment.”
Special populations require adapted approaches. Perinatal women, older adults, and people with co-occurring substance use disorders all benefit from evidence-based treatment options that account for their specific circumstances. For example, IPT is particularly well-suited for postpartum depression because it addresses the relational and role changes that often trigger or worsen symptoms.
If you are experiencing a crisis or your symptoms are worsening rapidly, telehealth therapy can provide same-week or even same-day access in many cases, which matters when waiting is not an option.
What most guides miss: The crucial mindset for success
Here is something we see consistently in clinical practice: people who follow a workflow but treat it like a rigid checklist often plateau. People who treat it as a living, adaptable framework tend to keep moving forward.
A workflow is a foundation. It gives you structure when depression is stealing your ability to think clearly. But the structure only works when you bring genuine engagement to it. That means advocating for yourself when something is not working, asking questions, and being willing to try a different approach without interpreting it as failure.
Personalized plans consistently outperform one-size-fits-all protocols in real-world outcomes. Behavioral activation, which simply means scheduling and completing meaningful activities even when you do not feel like it, is one of the most powerful tools in any plan. Digital tools can reinforce this between sessions.
California’s mental health landscape is rich with resources, but navigating it takes self-advocacy. The most successful outcomes we see come from people who blend expert guidance with their own knowledge of what they need. You can build that self-knowledge by tracking your moods, noticing patterns, and sharing them openly with your therapist. Explore mental health coping tips to build that habit between sessions.
Get expert guidance for your next step
Knowing the workflow is a powerful first step. Taking it with the right support makes all the difference.
At Revive Health Therapy, we work with adults across California who are ready to move from understanding depression to actively overcoming it. Our therapists use CBT, EMDR, and trauma-informed approaches tailored to your specific needs, whether you are in Walnut Creek, Oakland, or connecting via secure telehealth from anywhere in the state. We accept insurance and offer sliding-scale fees so cost is not a barrier. If you want to understand why seek psychotherapy or explore psychotherapy options in California, we have resources ready for you. When you are ready, contact a therapist today and take the next step toward recovery.
Frequently asked questions
How quickly can I expect to see improvement in depression symptoms with this workflow?
Most adults see a 20% symptom reduction by week 4 when following an evidence-based workflow, with 65 to 79% showing marked improvement by session 12 using validated outcome measures.
What if I don’t feel better after a few weeks of therapy?
If there is little or no progress by week 4 to 8, that is a clear signal to discuss switching therapy types or adding medication with your provider. No early response by that point should always trigger a treatment review, not continued waiting.
Is affordable therapy available for adults in California?
Medi-Cal covers evidence-based therapies including CBT and IPT for eligible adults, and county mental health plans provide additional options for those who do not qualify for Medi-Cal.
Can digital or telehealth therapy be as effective as in-person sessions?
Telehealth and digital CBT are comparable in efficacy to in-person therapy for most adults, making them a practical and clinically sound choice for busy or geographically remote Californians.
What makes a depression workflow evidence-based?
An evidence-based workflow uses structured screening tools like the PHQ-9, best-practice therapies such as CBT or IPT, regular outcome tracking, and timely adjustments when progress stalls.
Recommended
- Practical mental health coping tips for Californians – Revive Health Therapy
- Step by step therapy guide for Californians 2026 – ReviveHealthTherapy
- 7 Essential Mental Health Tips 2026 for Californians – ReviveHealthTherapy
- Depression Treatment: Evidence-Based Solutions That Work – ReviveHealthTherapy
- Best bereavement support options in California: 13 months free | Graceland Hospice Care Blog