Mindfulness therapy is often dismissed as just another word for meditation, but that misses the point entirely. In clinical settings, it’s a structured, evidence-based approach that helps people manage anxiety, depression, trauma, and emotional dysregulation through practical, teachable skills. If you’ve been curious about whether mindfulness therapy could work for you, or whether you can actually afford it in California, you’re in the right place. This article covers what mindfulness therapy really is, how it works, what the research says, its limitations, and how to access it affordably right here in California.
Table of Contents
- Defining mindfulness therapy: More than meditation
- How mindfulness therapy works: Key techniques and methods
- Evidence and effectiveness for anxiety, depression, and trauma
- Nuances, limitations, and who should avoid mindfulness therapy
- Getting started with mindfulness therapy in California: Access and affordability
- Affordable, evidence-based mindfulness therapy options at Revive Health Therapy
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Mindfulness therapy defined | It’s an evidence-based approach that teaches present-moment awareness and emotional regulation using structured clinical techniques. |
| Proven for anxiety and depression | Research shows mindfulness therapy can reduce anxiety and depression symptoms comparably to traditional therapy. |
| Careful screening needed | About one in four people may experience adverse effects, so professional guidance is important. |
| Accessible and affordable options | Californians can access mindfulness therapy affordably through telehealth, insurance, and sliding scale practices. |
Defining mindfulness therapy: More than meditation
Most people picture someone sitting cross-legged and breathing slowly when they hear “mindfulness.” That image isn’t wrong, but it’s incomplete. Mindfulness therapy, as practiced in clinical settings, is about training your attention, building acceptance, and developing present-moment awareness so you can respond to difficult emotions rather than react to them automatically.
The goal isn’t to empty your mind or eliminate negative thoughts. It’s to change your relationship with those thoughts. As mindfulness in therapy shows, the real power lies in learning to observe your inner experience without judgment, which directly supports emotional regulation and coping. According to HelpGuide, mindfulness therapy incorporates mindfulness practices to foster present-moment awareness and a nonjudgmental attitude, aiding regulation of thoughts and emotions.
Here are some common misconceptions versus what mindfulness therapy actually involves:
- Misconception: Mindfulness therapy is just guided relaxation. Reality: It’s a structured clinical intervention with measurable outcomes.
- Misconception: You need to meditate daily for it to work. Reality: Techniques are adapted to individual needs and schedules.
- Misconception: It’s only for stress. Reality: It’s used for anxiety disorders, depression, PTSD, chronic pain, and more.
- Misconception: It replaces other therapy. Reality: It’s often integrated into broader treatment plans.
- Misconception: Results are immediate. Reality: Most programs run 8 to 12 weeks for measurable change.
How mindfulness therapy works: Key techniques and methods
With the basics clear, let’s explore what happens in a typical mindfulness therapy session and the methods proven most effective.
The four major frameworks you’ll encounter are Mindfulness-Based Stress Reduction (MBSR), Mindfulness-Based Cognitive Therapy (MBCT), Dialectical Behavior Therapy (DBT), and Acceptance and Commitment Therapy (ACT). Each uses mindfulness differently, but all share a focus on awareness and acceptance. MBSR and MBCT are evidence-based programs utilizing meditation, breath work, body scans, and are adapted for group or individual therapy. Mindfulness therapy is also integrated into modalities like DBT and ACT, expanding its reach across different clinical needs.

| Method | Primary focus | Session format | Best for |
|---|---|---|---|
| MBSR | Stress and chronic pain | 8-week group program | General stress, chronic illness |
| MBCT | Depression relapse prevention | 8-week group or individual | Recurrent depression |
| DBT | Emotional regulation, distress tolerance | Individual and skills group | Borderline PD, self-harm, intense emotions |
| ACT | Psychological flexibility, values | Individual therapy | Anxiety, avoidance, life transitions |
A typical session might move through these steps:
- Breath awareness: Anchoring attention to the breath to settle the nervous system.
- Body scan: Slowly moving attention through the body to notice tension or sensation without judgment.
- Thought observation: Watching thoughts arise and pass without attaching to them.
- Sensory grounding: Using the five senses to stay present, especially useful for trauma responses.
- Reflection and integration: Discussing what came up and how to apply skills between sessions.
Pro Tip: Many therapists now adapt these methods for telehealth and group settings, so you don’t need to be in a specific city to access quality mindfulness-based care.
Evidence and effectiveness for anxiety, depression, and trauma
Understanding how these techniques work is one thing. Now let’s look at how well they hold up under scientific scrutiny.
Meta-analyses show moderate effects on anxiety (SMD approximately 0.48), depression (SMD approximately 0.38), and sustained benefits for relapse prevention. These aren’t dramatic numbers, but in mental health research, moderate effect sizes are clinically meaningful, especially when benefits persist over time.
Key finding: MBCT reduces the risk of depression relapse by up to 43% in people with three or more previous episodes, making it one of the most effective long-term tools for recurrent depression.
| Therapy type | Anxiety reduction | Depression reduction | Relapse prevention | Sustained benefit |
|---|---|---|---|---|
| Mindfulness therapy | Moderate (SMD ~0.48) | Moderate (SMD ~0.38) | Strong (MBCT) | Yes |
| CBT | Moderate to strong | Moderate to strong | Moderate | Yes |
| Standard care | Low to moderate | Low to moderate | Low | Variable |
Mindfulness therapy is effective for trauma and emotional regulation, though research confirms it is not superior to CBT or behavioral therapy across all conditions. That’s not a weakness. It means mindfulness therapy works best as part of a personalized plan, not a one-size-fits-all fix.
Key benefits supported by evidence:
- Reduced anxiety symptoms and worry cycles
- Lower rates of depression relapse, especially with MBCT
- Improved emotional regulation and distress tolerance
- Better trauma coping through grounding and body awareness
- Reduced physical symptoms linked to chronic stress
Nuances, limitations, and who should avoid mindfulness therapy
While mindfulness therapy offers real benefits, not every approach is risk-free or universally appropriate. Here’s what you need to know before starting.
One of the most important things to understand is that mindfulness therapy is not harmless for everyone. Research indicates that symptoms can worsen in approximately 25% of people, particularly those with trauma histories, OCD, or psychosis. The practice of turning inward can sometimes amplify distress rather than reduce it.
People who should approach mindfulness therapy with caution or avoid it without professional screening:
- Those experiencing acute psychosis or active hallucinations
- Individuals with complex trauma who haven’t yet established safety and stabilization
- People with severe OCD where introspection can fuel rumination
- Anyone in a mental health crisis who needs immediate stabilization first
There’s also a broader concern worth naming. Mindfulness has been heavily commercialized, with apps and wellness brands sometimes overpromising results. This can create unrealistic expectations and, in some cases, delay people from seeking the structured clinical support they actually need. The real impact of mindfulness is meaningful but requires proper clinical context to be safe and effective.
Pro Tip: Always consult a licensed therapist before starting a mindfulness-based program, especially if you have a trauma history or a diagnosed mental health condition. A brief screening can make the difference between a helpful experience and a harmful one.
Getting started with mindfulness therapy in California: Access and affordability
With a clear-eyed view of the pros, cons, evidence, and risks, you’re ready to take the next step toward finding quality, affordable support tailored to California’s resources.
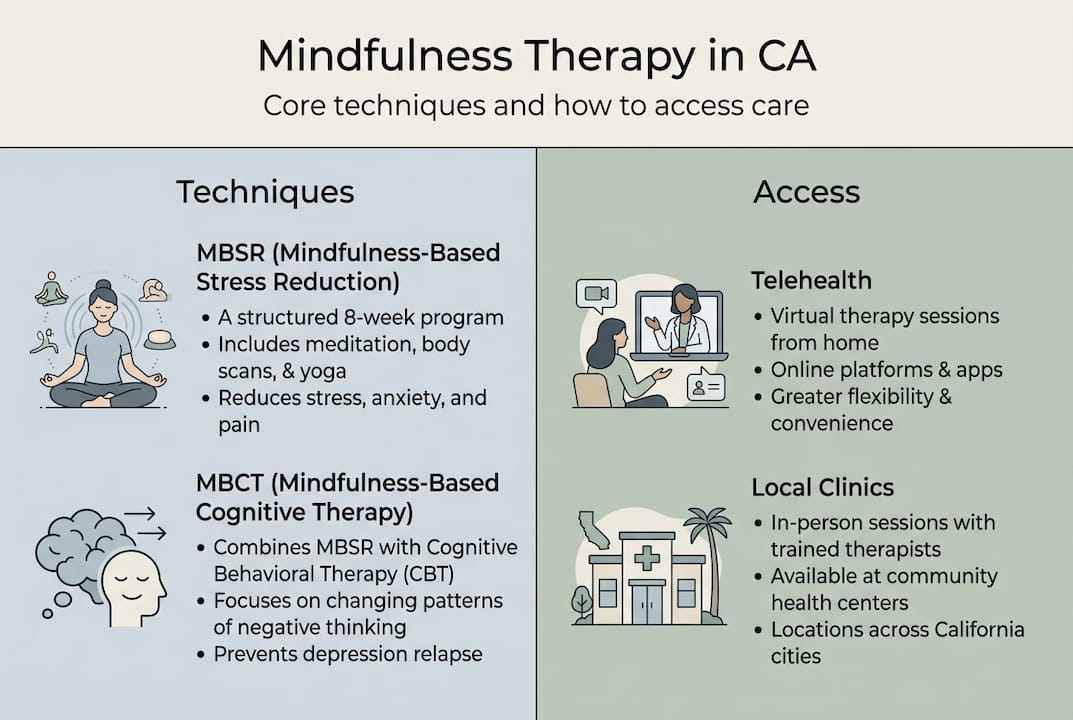
California has some of the most accessible mental health infrastructure in the country, including telehealth options, sliding-scale clinics, and insurance-covered services. Affordable online options, including platforms like BetterHelp starting around $65 to $100 per week and insurance-accepted telehealth, are available for Californians across the state.
Here’s how to find an affordable mindfulness therapist:
- Verify credentials: Look for licensed therapists (LCSW, MFT, PhD, PsyD) with specific training in MBSR, MBCT, DBT, or ACT.
- Check your insurance: Many California plans now cover mindfulness-integrated therapy. Review your insurance and therapy options before your first appointment.
- Ask about sliding-scale fees: Many therapists offer reduced rates based on income. Don’t assume you can’t afford it before asking.
- Explore telehealth: California residents can access licensed therapists statewide through secure video sessions, removing geographic barriers.
- Use trusted platforms: Research reputable services before committing.
Affordable options worth exploring:
- BetterHelp: Online therapy starting around $65 to $100 per week
- Open Path Collective: Reduced-fee sessions for individuals and families
- Community mental health centers: County-funded services with income-based pricing
- Revive Health Therapy: Sliding-scale fees, insurance accepted, telehealth statewide
For a broader look at what’s available, affordable mental health care resources in California are more varied than most people realize. You can also compare affordable therapy services to find the right fit for your budget and needs.
Affordable, evidence-based mindfulness therapy options at Revive Health Therapy
If this article has helped you see mindfulness therapy in a new light, the next step is finding a provider who can deliver it safely and effectively. At Revive Health Therapy, we offer evidence-based mindfulness-integrated care for anxiety, depression, trauma, and emotional regulation, with services available in Walnut Creek, Oakland, and statewide via telehealth mental health access.
We accept insurance, offer sliding-scale fees, and work with HSA/FSA plans to make quality care genuinely accessible. Whether you’re exploring why psychotherapy might be right for you or you’re ready to book your first session, our team is here to help you find the right fit. Reach out today for a free consultation and take the first step toward lasting emotional wellness.
Frequently asked questions
Is mindfulness therapy covered by California insurance plans?
Most California insurance plans now cover evidence-based mindfulness therapy, especially when integrated with telehealth or CBT services. It’s worth calling your provider directly to confirm your specific benefits.
How quickly can I expect results from mindfulness therapy?
MBSR is structured as an 8-week program, and many people report measurable reductions in anxiety and improved emotional regulation within that timeframe, though individual results vary.
Can mindfulness therapy make symptoms worse?
Yes, symptoms may worsen in about 1 in 4 people, particularly those with trauma, OCD, or psychosis. Professional screening before starting is strongly recommended.
Are there affordable online mindfulness therapy options in California?
BetterHelp and similar platforms offer mindfulness therapy starting around $65 per week, and many California therapists provide sliding-scale rates for those who qualify.
How does mindfulness therapy differ from standard meditation?
Mindfulness therapy is a structured clinical approach using techniques like thought observation and emotional regulation within a therapeutic relationship, while meditation is typically a personal, self-directed practice without clinical oversight.
Recommended
- Therapeutic modalities explained: 35% better outcomes in 2026 – ReviveHealthTherapy
- Role of Mindfulness in Therapy: Real Impact on Anxiety and Depression – ReviveHealthTherapy
- Practical mental health coping tips for Californians – Revive Health Therapy
- Why mental health accessibility in California boosts recovery 50% – ReviveHealthTherapy

3 Responses